High-resolution & high-sensitivity immuno-SPECT in oncology
Prof. dr. Otto Boerman, Radboud University Medical Center Nijmegen, the Netherlands
Otto Boerman Ph.D. is professor in Radiochemistry at the Radboud University Nijmegen, The Netherlands. His preclinical research focuses on radionuclide imaging and radionuclide therapy with radiolabelled peptides (RGD, CCK2R, GLP-1R, GRPR, a.o.) and antibodies (anti-CAIX, anti-CEA, a.o.). Otto is on the board of several international journals (including JNM and EJNMMI). He (co-) authored more than 420 scientific publications and is recipient of several prestigious international awards for innovating radiochemistry.
Can you explain what the research focus is of your group in Nijmegen?
“The main focus of my research group is the synthesis, optimization and characterization of new radiotracers for molecular imaging and radionuclide therapy of cancer. In our research we use high-end molecular imaging equipment to image and quantify in vivo behavior of the tracer in relevant animal models.
Currently, one of our key research topics is the development of molecular imaging techniques to evaluate anti-cancer therapy with immune checkpoint inhibitors such as antibodies against Programmed Death Ligand 1 (PD-L1). Tumors can escape immune recognition and attack by T cells by expressing PD-L1, because the interaction between PD-L1 with PD-1 on T cells are deactivated. Antibodies that block the interaction between PD-1 and PD-L1, such as nivolumab or pembrolizumab, have shown remarkable antitumor activity in cancer patients. Despite these promising results, not all patients respond to this type of treatment and there is an urgent need for a predictive biomarker. Several studies have suggested that tumor PD-L1 expression might be a prerequisite for response to anti-PD-1 and anti-PD-L1 targeted therapy. However, immunohistochemical analysis of PD-L1 expression as determined on archival tissue samples should be interpreted with caution, since PD-L1 expression may undergo changes due to alterations in the tumor microenvironment or previous treatment. Molecular imaging with radiolabeled anti-PD-L1 antibodies may overcome some of these limitations. It allows measurement of PD-L1 expression at time of start of therapy, of whole tumor lesions and their metastases, thereby avoiding sampling errors and thus misinterpretation due to intratumoral and interlesional heterogeneity. This may result in more accurate detection of PD-L1 expression and in vivo accessibility. It can potentially be used as biomarker to select patients for PD-L1/PD-1 targeted therapy, and it allows longitudinal monitoring of PD-L1 expression during disease progression and treatment.”
How do you use molecular imaging tools in your PD-L1 research?
“Molecular imaging with microSPECT/CT is of inevitable value in our studies. In this project we used an 111In-labelled anti-PD-L1 monoclonal antibody. We first determined the optimal imaging time point for imaging PD-L1 expression in mice by imaging mice with s.c. MD-MB-231 xenografts longitudinally during 7 days (Fig. 1).
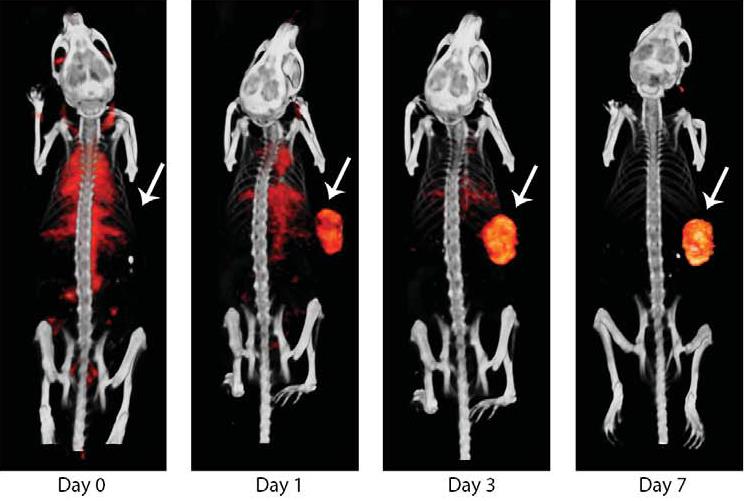 |
| Fig. 1. Longitudinal SPECT/CT of a mouse with subcutaneous MDA-MB-231 xenografts. Images were acquired at 4 time points after injection of 15.5 MBq 111In-PD-L1.3.1 (1.5 mg).1 |
To evaluate the potential of this tracer to quantitatively determine PD-L1 expression in tumors we acquired microSPECT/CT scans of mice with human breast cancer xenografts with various levels of PD-L1 expression. With the U-SPECT/CT system we determined the tumour uptake in these mice (see Fig. 2)”.
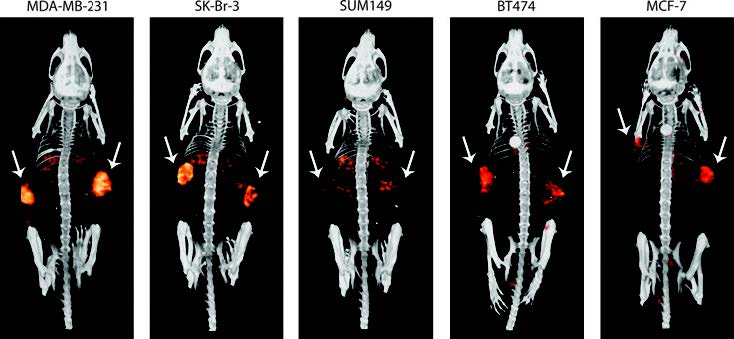 |
| Fig. 2. SPECT/CT scans of mice bearing subcutaneous breast cancer xenografts, with different PD-L1 expression levels, on both flanks (indicated with the white arrows). Scans were acquired 3 days after injection of 10 MBq 111In-PD-L1.3.1 (1 μg). Mean tumor weight was 99 ± 4 mg. 1 |
What is the added value U-SPECT/CT for your research ?
“At our preclinical imaging facility PRIME in Nijmegen we use the MILabs U-SPECT/CT system 4-8 hours a day, for a wide variety of molecular imaging tasks. Over the last years the U-SPECT/CT system has been used extensively with a wide array of SPECT tracers, labelled with radionuclides such as 111In, 99mTc, 125I and 177Lu. Recently someone found out that we have already published 35 full papers in peer reviewed journals using our U-SPECT/CT. I think this shows the value of a robust SPECT/CT system.”
References:
1Heskamp S, Hobo W, Molkenboer-Kuenen JD, Olive D, Oyen WJ, Dolstra H, Boerman OC. Noninvasive Imaging of Tumor PD-L1 Expression Using Radiolabeled Anti-PD-L1 Antibodies. Cancer Res. 2015
